David Fletcher, MD
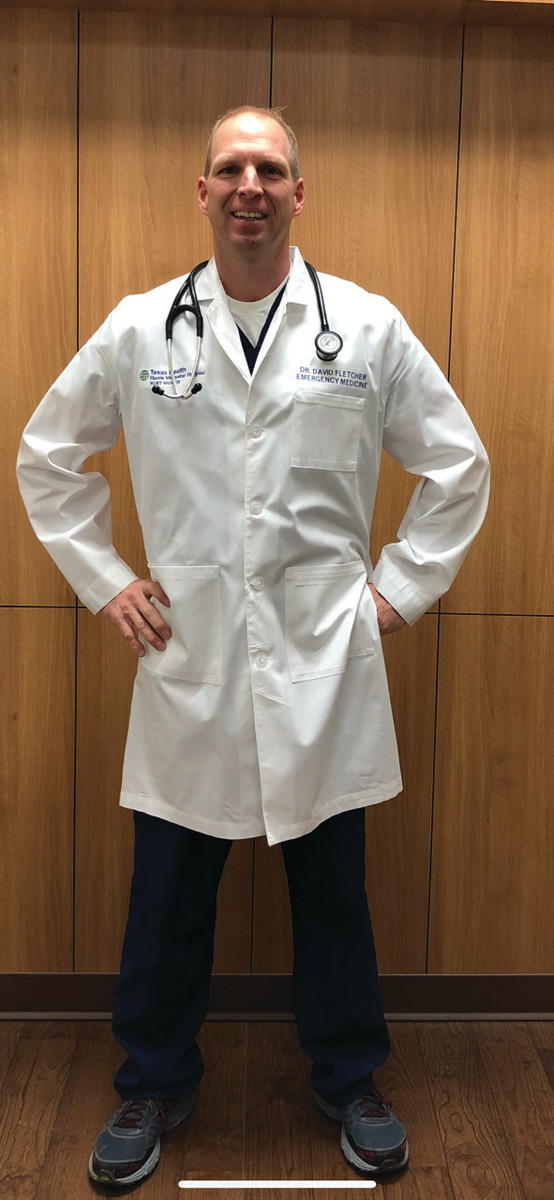
Emergency Medicine Physician at Texas Health Harris Methodist Hospital in Fort Worth, Texas
On hospital life: We’ve received quite a few patients who have the virus, but we’re still expecting more to come. Right now, my day is more spent in meetings and planning for worst-case scenarios—if we run out of ventilators or ICU space. All of that involves lots of meetings done on conference calls with all different specialties in the hospitals and administration. The other half the time, I’m working. We’re seeing a fair number of people with the virus, from not very sick people to people on ventilators. The rest of the volume—because people aren’t driving much or getting injured—the volume is way down.
On roping: I haven’t been roping at all. I slowed down a little before COVID-19 started, so it hasn’t been a huge change. I’m not practicing as much, so I feel like, for me to go to compete, I’ll have less partner and less practice. And that isn’t how I like to do things. So right now I haven’t done any of it. I’m either in it all the way or not in it. Right now I’m not too in it. That could change tomorrow, though.

[Shop: COVID-19 Prevention Supplies]
Milcoast 3-Ply Layer Disposable Earloop Face Masks
(As an Amazon Associate, we earn from qualifying purchases made through affiliate links.)
Jane Hedeman, RN


City Hospital Emergency Care Center, Arlington, Texas
On hospital life: COVID-19 has changed all of our direct patient care. If you have a fever at all, a cough, anything—unless you’re completely ruled out—we can’t touch that patient without full PPE (personal protective equipment) on. We have no visitors allowed in the building, except for children. It truly has changed how I personally provide care. I am a really, really hands-on nurse, so it has cost me my personal touch with my sick patients, which makes me pretty sad. I was a nurse during the AIDS epidemic, and I still was able to have that personal touch, and now I have lost it. Personal touch is vital to really sick patients and for us who care for them. Providing care to really sick patients has always been when I’m at my best.
On roping: As the grandma, I have the best job at Mathews Land and Cattle. I used to be the secretary, but Kenna and Chris (Francis) had Karstyn; I have the best job watching her. We’re buddies. It’s difficult spending so many weeks away from her. Karstyn has a whole herd of cows, and we set up a ranch everywhere we go. I was mooing like a cow or a bull, and a man walked by and said “Only a grandmother would moo like a cow for her granddaughter,” and he’s right—I get to spend so much time with her usually, and it’s been hard being without her.

Jason W. Stoneback, MD
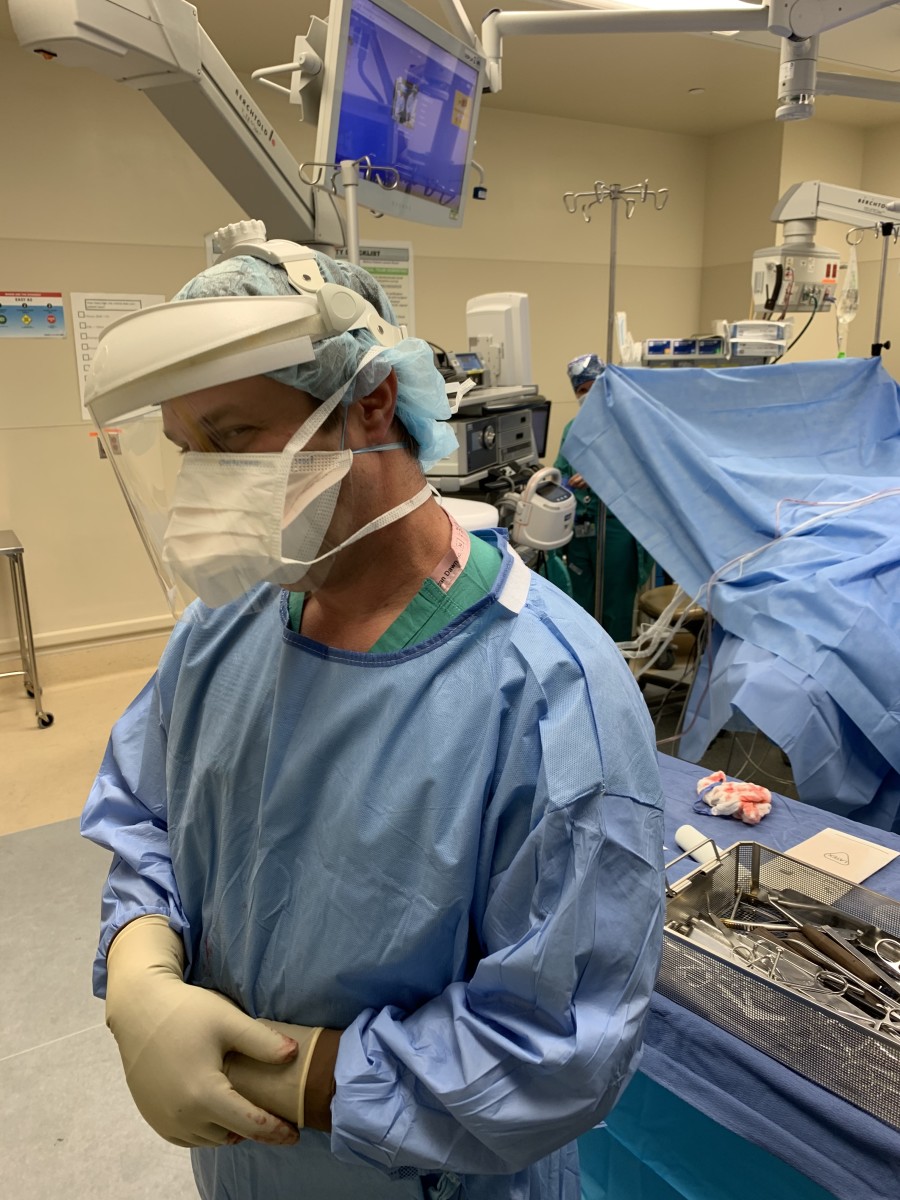
Vice Chair and Chief, Orthopedic Trauma and Fracture Surgery Service,
Department of Orthopedics, University of Colorado School of Medicine
On hospital life: When we recognized the COVID-19 surge was coming, department leadership made the decision to stop all elective surgeries to preserve PPE and decrease patients in beds. We had to quickly triage all the patients we had scheduled for surgery and see who was absolutely critical. From there, I immediately developed a disaster management plan for the department, especially as a level-one trauma and burn center, because we still have patients who need cared for. We broke our larger team of surgeons into small groups who work one week on, two weeks off, so in case one of us gets infected, we still have others who can carry on. And if we contract COVID-19, the two weeks off will hopefully allow us to recover and rejoin the fight. During crises like these, our entire physician work force has been converted to a where-we’re-needed team. As an orthopedic surgeon, I’m not on the front lines like the ICU and ER doctors. But physicians have to become doctors first, and that means some of our providers are working in the ICU to help with patients with COVID-19.
On roping: When I’m not at the hospital, I’m on the phone in meetings or doing tele-health. But I’m very fortunate to live where I live in Fort Lupton, Colorado. I rope with my wife, so in between meetings I rope the dummy, and when some of the stuff falls off for the day, we’ve been roping the steers and I have my phone with me no matter what. I’m lucky to have the greatest wife in the world who makes that possible.

Kara Ruthruff, CCRN
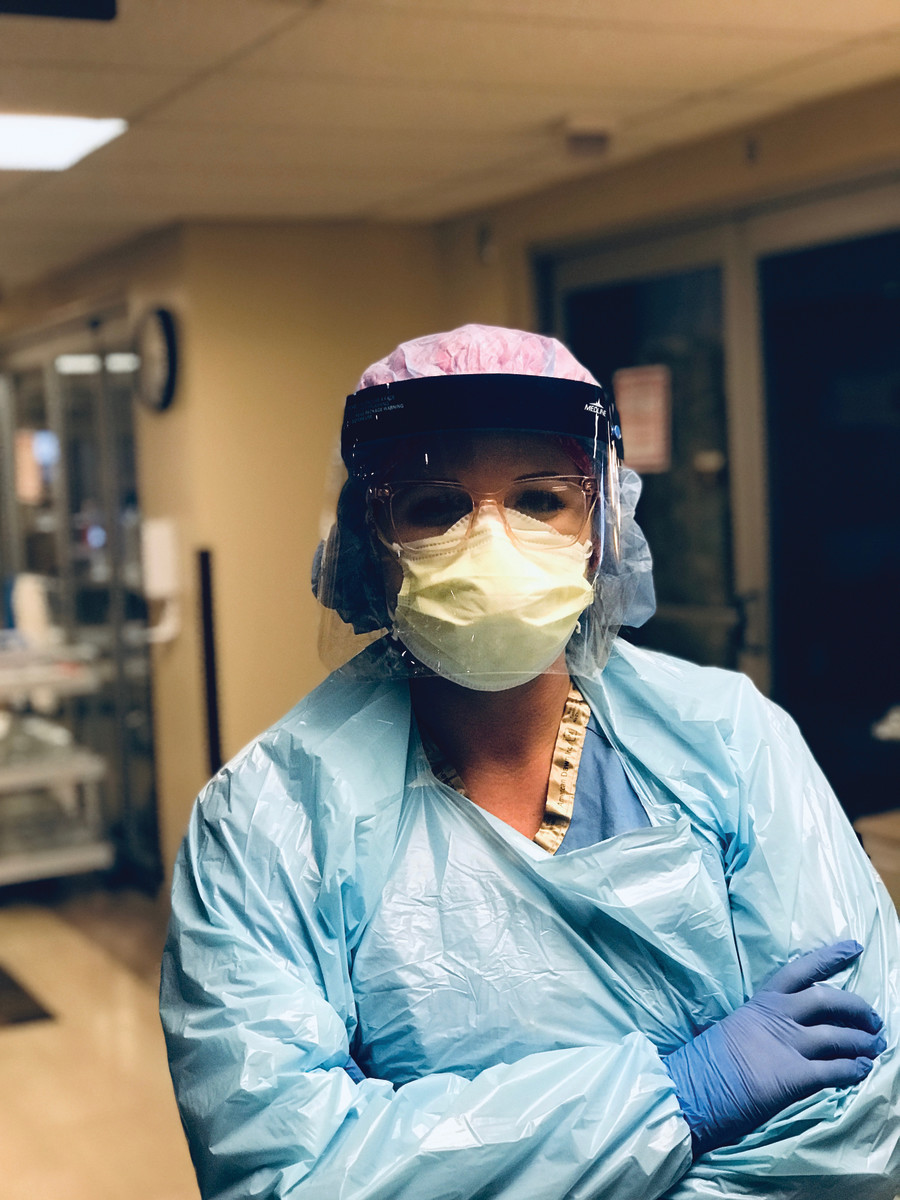
Critical Care Nurse, The Medical Center of Aurora, Colorado
On hospital life: It’s been 100% a war zone. It’s nothing I’ve experienced in my 10 years as an ICU nurse. We’re all trying to survive and have our patients survive. We’re opening up areas that were never meant for ICU patients all day. We’re putting people where we can, running around trying to keep people alive. I’m working three days a week, 12-hour shifts. But they’ve asked me to work overnights because we’re so critically low on staffing.
One day, I was getting a report from the night nurse on one patient that had been intubated with COVID for two weeks, when a whole group of people pushed a patient into one of my open rooms without calling or telling me. He’d been on the COVID-19 medical floor, but they said, “He needs to be intubated immediately,” and sent him to me in the ICU. He was COVID positive, and his wife was two doors down also on life-support and COVID-19 positive. He begged me to help him, but he also begged me to give his wife the ventilator if we had to choose. We intubated him, and I spent four hours trying to keep him alive after that and didn’t leave his room. And I went home and prayed I was not the last face he was going to see.
On roping: My down time is 100% what I look forward to with the kids and my husband and the horses. Whether we’re pulling the Hot Heels around on my day off or at night after work, or I’m riding my 3-year-old. That 3-year-old is keeping me sane.

Kersti Passig, RN

Emergency Medicine, Alta Vista Regional Care Hospital, Las Vegas, New Mexico
On hospital life: At first, I was skeptical. Even as a nurse, I thought it really wasn’t that bad. My mindset changed as it spread in the U.S. I don’t feel scared for myself, but I feel scared for my hospital and my patients and our staff. We’re so rural, and we usually transfer patients who are too critical. But hospitals where we usually transfer our critical patients to are filling up. As long as we take our precautions, we’ll get through. The PPE rationing has been our biggest change. Now we’ve been given one N-95 mask. We keep them in brown paper bags, and we’ve got the cloth masks that everyone is making for us. Normally that’s a no-no, but it’s what we have. We’re just getting rooms ready, bags of supplies ready in case we get a case. Luckily, we haven’t had to see a patient and go in blind. We’ve definitely been extremely slow, which is honestly scary because it feels like the calm before the storm. In the whole realm of things, it’s good our community is doing a really good job of staying home. Our town doesn’t have an urgent care, so we’re used for everything. But those people have been staying home. We see some non-emergent things, but for the most part it’s been a waiting game.
On roping: I feel like I’ve roped more now than I ever have because there’s no ropings to go to. They’ve been breaking in steers every day. I’ve gotten to practice and I have nowhere to go! Rarely do I get to practice with my husband (BFI champ Cade Passig) and Chris (Francis) and Kenna.










